What is Tay-Sachs Disease?:
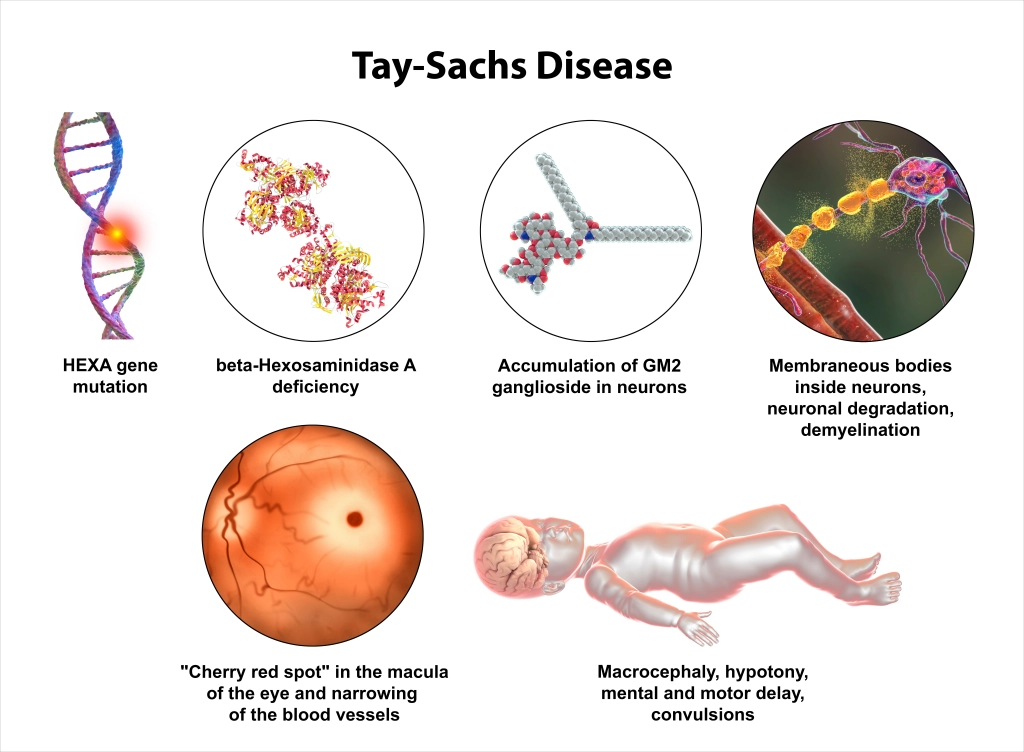
Tay-Sachs disease is a neurodegenerative orhpan disease caused by a severe deficiency of the enzyme b-hexosaminidase A. This enzyme is meant to break down fats in the brain, without it, these fats begin to accumulate in the brain, as well as other organs. This progressive accumulation corresponds to the progressive dysfunction of the nervous system. Being a lysosomal storage disease, an individual with Tay-Sachs disease lacks the means to properly break down large molecules, like fats, in the lysosomes of their cells. This causes fats and carbohydrates to build up in the lysosomes, causing these cells to eventually die, which will trigger and inflamatory response, causing further damage to the surrounding tissues.
There are three different types of Tay-Sachs disease, the type being determined by when the disease was onset in the individual. Infantile Tay-Sachs disease begins to present symptoms around 6 months of age. These symptoms include worsened vision, exaggerated responses when startled, and a loss of acquired skills. By age 2, the individual may begin to have seizures, leading to early death around the age of 5. Juvenile Tay-Sachs disease presents itself around the age of 5, while late-onset Tay-Sachs disease presents itself when when the individual is in their teens into adulthood. Tay-Sachs disease is an autosomal recessive disorder and is thus inherited as such; however, the time of onset of Tay-Sachs disease, and, thus, the type, is determined based on how much residual enzyme activity is present in the individual’s cells.
Symptoms:
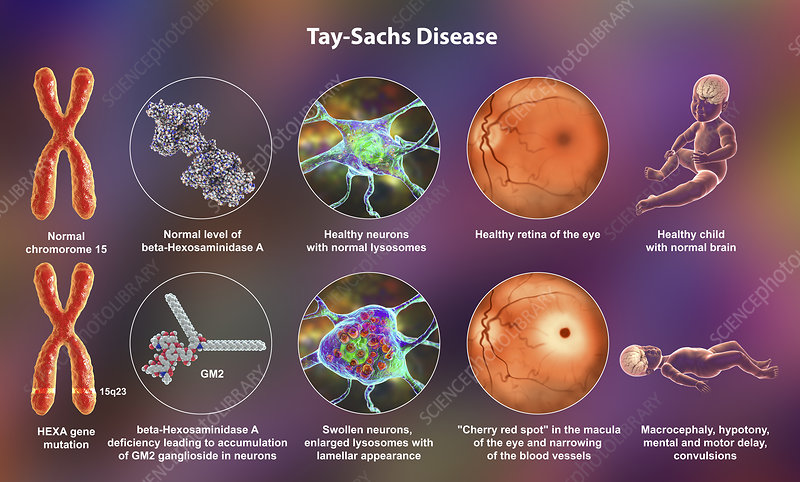
Infantile Tay-Sachs Disease:
Infantile Tay-Sachs disease results from the near complete lack of b-hexoaminidase A enzyme activity, causing extreme cognitive deterioration. Initial symptoms tend to develop around 3-6 months of age, including muscle weakness, twitching of the muscles, exaggerated responses to being startled. This also includes a heightened reaction to noise. Between the ages of six and ten months, infants with Tay-Sachs disease will fail to gain motor skills, no longer make eye contact, have unusual eye movements, be irritable, grow slowly, have weakened muscles and lose muscle tone, experience loss of vision, have muscle spasms, have slow and stiff movements, and a loss of previously acquired skills. Another characteristic symptom of Tay-Sachs disease is the formation of a red spot on the retina caused by the accumulation of undigested material, contrasting the background. This cherry red spot is reported in 90% of those with infantile Tay-Sachs disease.
As those with infantile Tay-Sachs disease age, worse symptoms are likely to develop. These symptoms include seizures, difficulty swallowing, loss of vision, paralysis, progressive hearing loss, confusion, disorientation and/or deterioration of intellectual abilities. Once the individual with infantile Tay-Sachs disease reaches three to five years old, their condition becomes far more life-threatening, as the child may become unresponsive to their environment as well as developing aspiration pneumonia, which can lead to respiratory failure and even death.
Juvenile Tay-Sachs Disease:
Between the ages of 2 to 10 years, juvenile Tay-Sachs disease can develop. The individual will display symptoms including clumsiness, difficulty controlling bodily movements, loss of speech, loss of life skills, and loss of intellectual abilities. These children may also experience the degenerative loss of retina cells, causing these children to become less aware of or interactive with their environment. Then, around 15 years of age, life-threatening symptoms can occur.
Late-Onset Tay-Sachs Disease:
Late-onset Tay-Sachs disease can present itself anywhere between the teen years into adulthood. Late-onset Tay-Sachs disease progresses far slower than any other variant of the disease. It is also possible for members of the same family to express symptoms at different times and at varying intensities. Most symptoms include muscle weakness, clumsiness, muscle twitches, cramping, weakness. As a result of their muscle weakness, most individuals with late-onset Tay-Sachs disease must lock their knees in order to support their own weight, if they do not, they may need a device or a cane to support them when walking. Later-developed symptoms may include difficulty swallowing, tremors, and slurred speech. The symptoms can eventually develop into psychiatric mania, acute depression, and/or psychosis, requiring psychiatric care. Memory issues and cognitive impairments are also likely to develop later on in the course of the disease.
Causes:
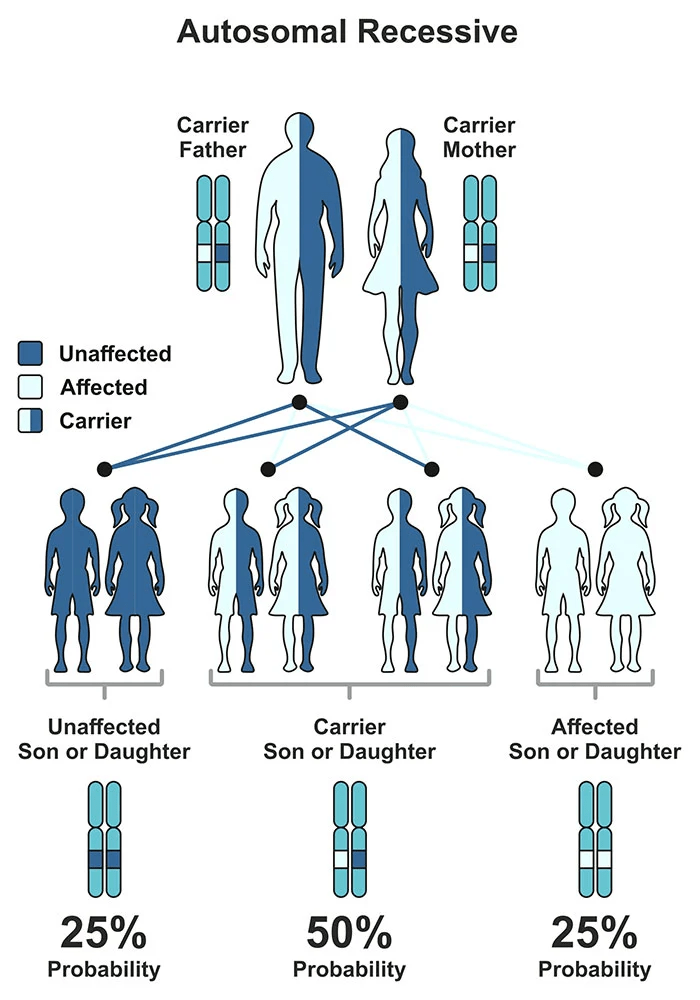
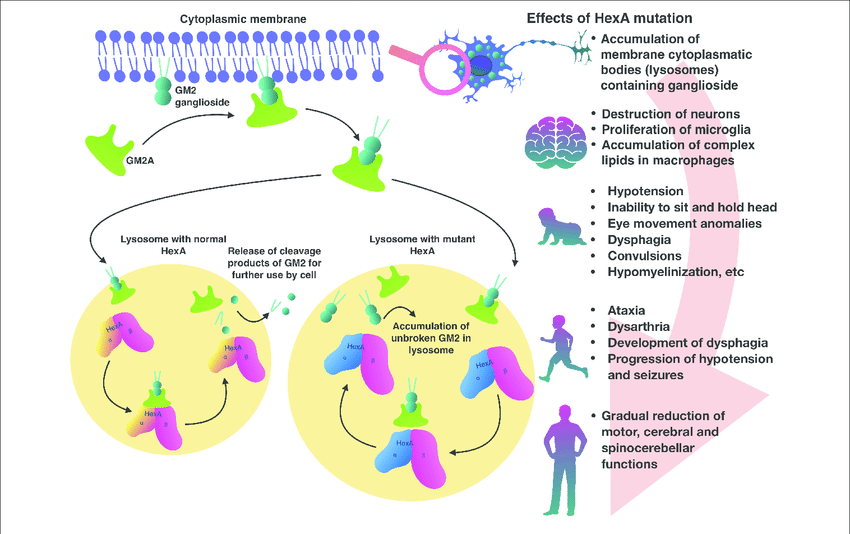
Tay-Sachs disease is the result of a malformed or faulty hexosaminidase subunit alpha (HEXA) gene, affecting several organ systems in the body. By a person inheriting two altered copies of the HEXA gene, which contributes to a deficiency of the hexosaminidase A enzyme, causing the body to be unable to break down certain fats within the cells of the body. This abnormal accumulation in the brain results in serious deterioration of the central nervous system.
Infantile disease is characterized by a complete lack of the hexosaminidase A enzyme; however, individuals with juvenile and late-onset Tay-Sachs disease still present some enzyme activity, which helps to explain why these two variants progress at a much slower rate and have less intense symptoms. Since Tay-Sachs is an autosomal recessive disorder, an individual must have both alleles to have the disease, as with one they will only be a carrier. This also means that if two carriers produced offspring they possesses a 25% chance to have a normal baby, a 50% chance to have a carrier child, and a 25% chance to have a child with Tay-Sachs disease.
Diagnosis:
Typically, blood tests are given to evaluate the enzyme levels in an individual. Molecular genetic testing is also widely used to diagnose Tay-Sachs disease as it reveals the whole of the genetic sequencing and confirms the concentration of enzymes. Prenatal diagnosis is also possible, and it is rather similar to genetic testing, only it uses chorionic villus samplings. This is the removal of some tissue from the placenta for genetic testing. Amniocentesis is the removal of some fluid surrounding the unborn fetus for testing. It is most commonly used when Tay-Sachs disease has been reported in the family.
Carrier testing is also available, requiring a blood sample to determine if an individual carries the one Tay-Sachs-causing gene. It is thoroughly recommended that individuals with Jewish descent are tested for being a carrier before becoming pregnant. If a couple should determine they are both carriers, options like in vitro fertilization and adoption are encouraged substitutes for starting a family. However, carrier couples are suggested to consult a genetic counselor on these choices.
Treatment:
There is currently no treatment for Tay-Sachs disease, so treatment is directed at helping a patient with their specific symptoms. Many specialists may be required depending on the different symptoms being experienced by the individual with Tay-Sachs disease. Since infants with Tay-Sachs disease may have difficulty feeding, nutrition and hydration monitoring is crucial. Feeding tubes may also be helpful in preventing food or liquid from entering the lungs. Individuals can also take anticonvulsants to treat their seizures; however, they don’t work on everyone.
How You Can Make an Impact:
Without proper research, funding, and support for continued studies and clinical trials to determine possible cures or legitimate medicines for the disease, many more children and adults will go on to develop Tay-Sachs disease. If you can, please donate here! If you are unable to donate, consider volunteering your time by raising awareness for this rare disease. If you’re interested in learning more about Tay-Sachs disease, donation opportunities, or the progress being made on potential treatments, visit the National Tay-Sachs Disease and Allied Diseases Foundation! The National Tay-Sachs Disease and Allied Diseases Foundation strives to “provide… individuals and families with connection, resources, and individual support… to meet [the] changing needs of families and shifts in research and industry.”
Let’s keep spreading awareness! – Lily
References:
Renna, K., & Toro, C. (2025, January 27). Tay Sachs Disease – Symptoms, Causes, Treatment | NORD. NORD (National Organization for Rare Disorders); NORD. https://rarediseases.org/rare-diseases/tay-sachs-disease/
Leave a comment